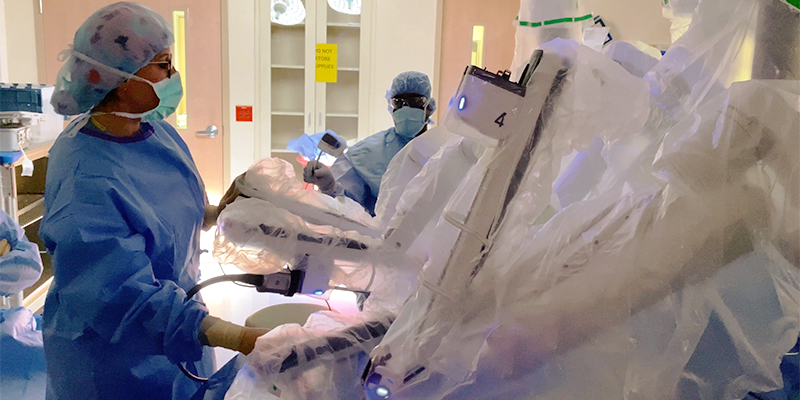
Robotic surgery has no stronger advocate than this Florida physician — an expert in the ever-advancing field.



Marina Gorelik, D.O.
Director
Robotic Center of Excellence
Kendall Regional Medical Center
Miami, Fla.
Growing up in the small city of Mohyliv-Podilskyi, Ukraine, Marina Gorelik, D.O., would often accompany her grandfather, an endocrinologist working as a primary care physician, as he saw his patients. That experience stayed with her, even after her family (including her grandparents) immigrated to Los Angeles, Calif., in 1996 when she was only 10 years old.
After graduating from the University of California, Santa Barbara, and earning her medical degree at Touro University Nevada in Las Vegas, Nev., Dr. Gorelik relocated to Florida for her residencies — and never left. Today, at just 34 years old, she is the director of the Robotic Center of Excellence at Kendall Regional Medical Center in Miami.
Q: When did you first become involved with robotic surgery?
A: I was introduced to it in medical school. I rotated with a general surgeon who was using it in its early stages. It wasn’t really available for a lot of complex operations, but we were doing gallbladders and hernias. I was enticed by how amazing the visualization was and how precise it allowed the surgeon to be, especially in comparison to standard laparoscopy, and by being able to perform the most precise types of surgery in a minimally invasive fashion. In residency, I took every robotic general surgery case that I could, and my passion and interest grew. We were starting to perform the more complex operations like colorectal surgery, and it became clear why this technology is so extraordinary.
Q: How would you define robotic surgery?
A: It’s a complex surgical tool. The advances in the software and visualization — the instruments we use — allow for a lot more complexity. Minimally invasive surgery encompasses both laparoscopic and robotic laparoscopic surgery. [Robots] are an extension of the surgery that we are able to do, using instruments that go through small incisions; the instruments are attached to arms that we control completely on the inside from a console away from the operating table.
Q: Could you explain the “human element” of this technology?
A: The robot doesn’t have any autonomy, but it does perfect a lot of things that humans can do. For example, high-definition vision and perfect depth perception. Even though we control the instruments, they have articulation. Through tiny incisions they can move like the human wrist. You don’t have to have your whole hand in the abdomen. What that enables is getting really close and seeing vessels and nerves and protecting them, and even being able to suture the smaller structures. With the robotic system, we can also [access] areas in the abdominal cavity — such as the pelvis or near the diaphragm — that would be very difficult to reach in an open fashion. Those surgeries use a special gas to lift the abdominal wall out of the way so we can see and manipulate the organs. The advantages for the patient are huge.
Q: What about the advances being made in this field?
A: I’m very excited about the new instruments. We’re seeing this every year. We are already doing a lot of complicated surgeries with this platform, but I think it will just get better in the sense that the instruments will allow us to have shorter operating times. I think it will be adopted by other surgical specialties as well.
With the robotic system we can access areas that would be very difficult to reach in an open fashion. The advantages for the patient are huge.— Marina Gorelik, D.O.
Q: Do advances in robotics happen incrementally or on a larger scale?
A: The system we use has made small changes that make a huge difference, but the principle behind it has been consistent. There’s been a rapid rise in the use of this technology, and the organization has listened to surgeons to optimize it. Visualization got better; setup is faster and easier. There haven’t been such significant changes to the systems that you would have to retrain completely, but rather special adaptations have been created that make surgery easier and instruments that function better.
Q: What are the limitations?
A: The main issues now are availability and accessibility. At Kendall Regional Medical Center, we’re very lucky that we do not feel that as much. We have six systems, and we’re almost at the point of having 24/7 access. But this technology requires space and a specially trained team — not just a surgeon, but also nurses, surgical techs and assistants. Sometimes it’s difficult to have all the stars align. The solution — and we’re getting there, at least in Florida — is that everybody has to be trained.
Q: You’ve been with Kendall since your residency. Why has this been such a good fit?
A: I grew up here. I have basically seen our mission play out, and I love the way we take care of patients. It just matches my goals and principles.
HCA Healthcare has more than 625 robots operating in 150+ facilities. Our robotic technology covers 15 surgical specialties across 15 suppliers of robotic systems.