Post-2020, elementary schoolers across the United States wash their hands more deliberately. Standing on a stool in front of the sink, waiting for the water to get warm, they prepare to sing the ABCs or maybe the song “Happy Birthday to You” twice — their choice, teachers say. What’s important is 20 seconds of scrubbing.
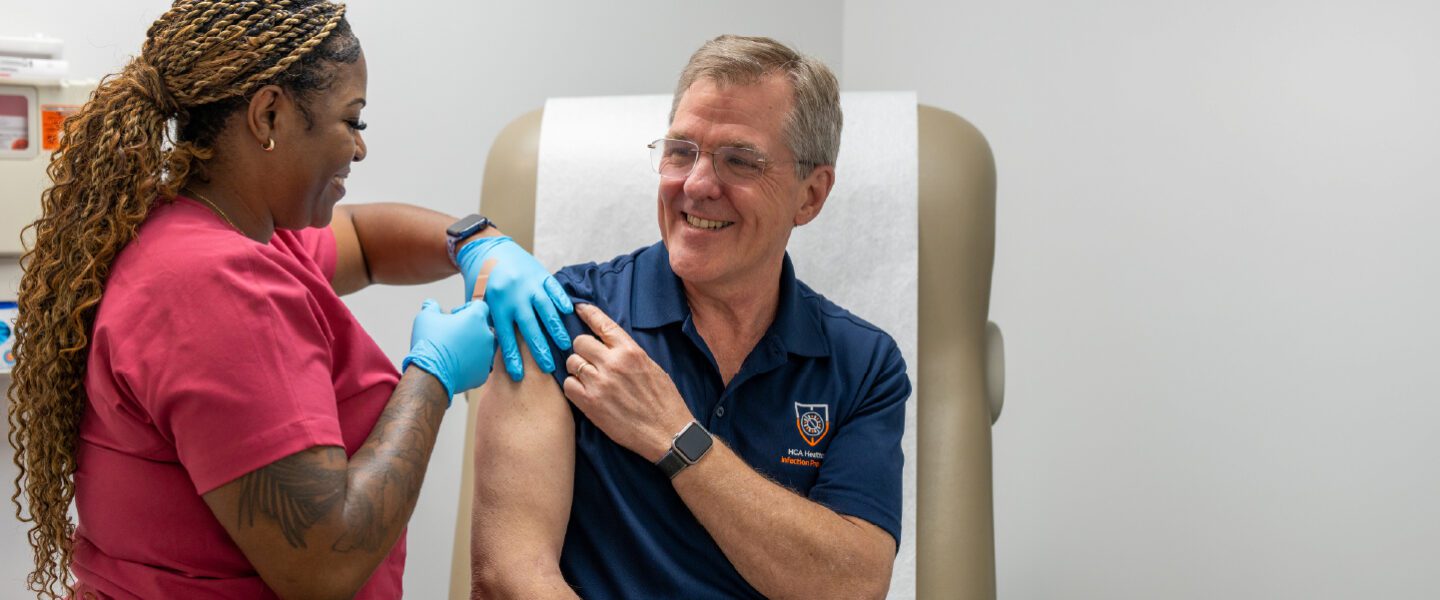
Healthcare professionals have long known what the COVID-19 pandemic revealed for everyday Americans. “I think people understand that hand hygiene is important for preventing infection; It’s something we’ve been taught since grade school,” says Chief Epidemiologist Ken Sands, MD, MPH. “But people may not appreciate what that means if you’re a nurse, for example. Nurses have to perform hand hygiene every time they enter and leave a patient’s room. That means they are washing their hands hundreds — if not thousands — of times a day.”
Parents and teachers can attest to the ripple effect of viral and bacterial infections during cold and flu season. But in healthcare facilities, the stakes are even higher.
“Our buildings are busy and complex, and people are sick, so the opportunity to spread infection goes with the territory,” says Dr. Sands. “It is important to protect our whole community — anybody who interfaces with our facilities — including patients, employees and visitors.”