Dr. Steven Rothenberg’s pioneering surgical methods have helped save some of the youngest and sickest patients, and have helped make a name for Rocky Mountain Hospital for Children.
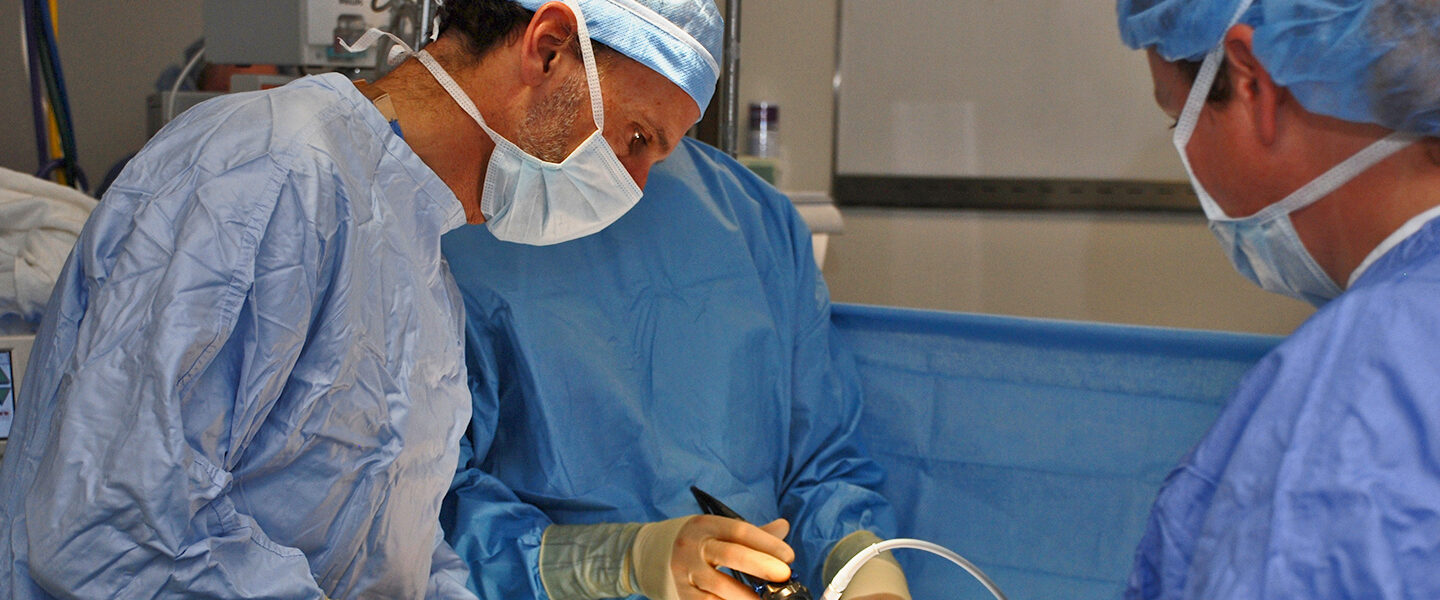
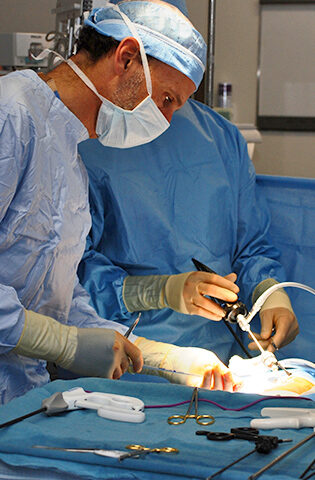

Steven Rothenberg, M.D.
Chief of Pediatric Surgery
Rocky Mountain Hospital for Children
Denver, Colo.
Last winter, Steven Rothenberg, M.D., chief of pediatric surgery at Rocky Mountain Hospital for Children in Denver, made history by performing a successful procedure on an infant, repairing what’s known as esophageal atresia. The birth defect occurs when part of the esophagus — the tube that connects the mouth to the stomach — does not develop properly.
Dr. Rothenberg used minimally invasive techniques he has helped develop, attaching the baby’s esophagus only 11 months after she was born.
“She is the smallest baby to have ever survived with this defect,” he says.
The effort to save her life involved three separate surgeries due to the wide gap in her esophagus. She suffered post-operative complications following the first two procedures in Denver, requiring lengthy recoveries and preventing her parents, Kayla Hatch and Victor Jacobo, from taking Baby Harper, as she came to be known at the hospital, back to her Nebraska home some 250 miles away.
“She was so sick,” Dr. Rothenberg said in an interview this past summer. “About six weeks after [the procedure], we were able to let her go home. I [recently] saw her and she looks phenomenal.”
Her remarkable recovery is just the latest milestone in the pioneering career of the 63-year-old surgeon.
“I’m very lucky,” he says. “Sometimes the best things that happen to you are pure luck. I thank the stars every day that I ended up doing what I’m doing.”
Q: What attracted you to pediatric care?
A: I had no intention of doing pediatric surgery. As a general surgery resident, I rotated on the pediatric surgery service. I was really fascinated by the different disease processes kids have, these complex congenital problems that babies are born with that you have to figure out how to fix.
Kids have no self-inflicted diseases. It’s not because they eat too much or drink too much. I really enjoyed being around the kids, so I decided to give it a try and get into a pediatric surgery fellowship. It was very much a surprise to me. I thought I was going to be a thoracic surgeon.
Q: How gratifying is your work?
A: It’s incredibly rewarding. Obviously, those of us in healthcare want to help our patients get better. But when you help a baby or a child, you affect the entire course of their life.
To see a baby — who might not otherwise survive — grow and thrive and become a fully functioning, happy kid is really incredible.
I have this book my children put together for my 60th birthday called “Thank You,” Dr. Rothenberg. It has pictures and messages from all these kids from the time I took care of them when they were babies, and many of them are adults now.
It’s incredibly special to have that kind of lifelong impact on these kids and their families. The parents are always scared to death when their kids are sick, and it’s a terrible time. If you can help make [the kids] better, the families are incredibly grateful. So yeah, it’s a great job.
Q: You’re known for minimally invasive procedures. What does that entail? And why is it important?
A: When we operate on a baby or a small infant with open surgery — a standard thoracotomy incision — there’s a high incidence of chest wall abnormalities, scoliosis and muscle girdle weakness in the shoulder.
I’ve spent most of my career trying to minimize the morbidity of those incisions. That’s why doing everything in a minimally invasive fashion becomes important, because we use just a couple of tiny incisions to go between the ribs, and we don’t cut any muscles.
As the kids grow, these little quarter-inch incisions nearly disappear, and they get normal chest wall development. There are also the initial benefits of less pain and [shorter] recovery. We have kids coming from all over the world to get lung and esophageal surgery.
Q: Which is why Rocky Mountain is considered a leader in this field, correct?
A: We use minimally invasive surgery on babies probably more than any other institution in the world. Before the pandemic, we would always have four or five visiting surgeons in the OR, mostly from [overseas], to learn these new techniques.
Q: What role does your team play?
A: No one person can take care of [surgery] this complex. We have an incredible team, and it starts with the neonatologists — the doctors who take care of these very sick, severely premature babies. Then there are the nurses and the advanced-care practitioners who work with them. I have an incredible OR crew, from the nurses and the techs to all the support systems.
It’s very important for everyone to recognize that Harper would not have survived, and thrived, without the hundreds of people who took care of her. It’s the hard work of the bedside nurses and the practitioners that kept her alive. The kudos go to all of those people, all the ancillary staff , the respiratory therapists, the nurses, the practitioners, the radiologists, everybody who helped do all the things we needed to do. It was a huge team effort.
Q: What do you see on the horizon?
A: Even though we do all of this surgery minimally invasively, most of [these procedures nationwide] aren’t done that way. I’m spending a lot of my time now trying to teach others. I was recently in Sweden and Israel teaching and doing cases. But I would love to be able to help surgeons overcome the hurdles of doing this.
More and more surgery will be done this way; the equipment keeps getting better, the imaging keeps getting better. There’s a lot we can do.